I think probably the first “real” counseling point any pharmacy student learns is “Don’t drink alcohol with Flagyl!” If it’s not the first thing, it’s easily the second or third. In fact, I’ve seen this hand-written on prescription labels for added emphasis, even though the auxiliary labels that print out already say it. You don’t often see “Take with food” hand-written, even though it would probably provide more real-world benefit to the patient than the standard “Don’t drink alcohol” mantra.
“Heresy!” you shout. Well, hear me out…
You see, there’s almost no data to support the assertion that alcohol and metronidazole combine to create a disulfiram-like reaction. It’s crazy, I know. How could this age-old advice be wrong? The reason this is drilled into pharmacy and med students’ heads is because the conventional wisdom is old. It got here because “everyone knows” that ethanol + metronidazole = A Bad Time. Even though there’s no meaningful evidence to support this conclusion.
Regular readers know my distaste (hah!) for metronidazole. In fact, I missed out on my best friend’s 21st birthday drunkfestcelebration because of it. As it turns out, I missed out for naught. Alas.
Exhibit A is a meta-analysis of published anecdotes, “Do Ethanol and Metronidazole Interact to Produce a Disulfiram-Like Reaction” published in The Annals of Pharmacotherapy. Exhibit B is a double-blind, placebo-controlled study out of Finland, also published in TAOP entitled “Lack of Disulfiram-Like Reaction with Metronidazole and Ethanol” which is a bit more science-y and a little less meta-analysis-y.
This is a long entry, so here’s a ToC.
Bits and bobs from Exhibit A (Back to top)
The first account of a metronidazole-ethanol interaction was noted in 1964. At that time, folks wondered if Flagyl could be used to curb alcohol abuse. A sort of proto-Antabuse, if you will. 8 of 17 studies found it to be marginally effective. But only marginally, and only 2 of the 8 positive studies were double-blind, and these 2 studies were statistically significant only when dropouts had been excluded.
My commentary after each quote.
revealed six case reports involving a total of eight patients. Tunguy-Desmerais reported on a two-year-old child taking acetaminophen and amoxicillin for pharyngitis. After a febrile seizure, ulcerative gingivostomatitis was diagnosed, phenobarbital–vitamin B6 syrup was added, and oral metronidazole was started. The next evening, the child was flushed but not febrile and, because both the analgesic and phenobarbital–vitamin B6 syrup contained ethanol, a metronidazole–ethanol reaction was considered likely.
I’m not an expert in pediatric liver function, but I do know that it takes longer for children to metabolize EtOH than it does for an adult. And the flushing is certainly a side effect of plain old alcohol consumption. Going right for the metronidazole-ethanol “reaction” seems a little too convenient, and more than a little irresponsible.
Another report involved three patients: a woman prescribed rectal metronidazole following hysterectomy, who became nauseous, pale, and dyspneic 36 and 60 hours postoperatively and was discovered to have taken a large amount of whiskey just prior to each episode; an 18-year old patient being treated with amoxicillin and metronidazole for pelvic inflammatory disease who experienced nausea, flushing, and headaches each evening after drinking ethanol; and a man who, after a 1g dose of metronidazole and a shared bottle of wine at his evening meal, vomited violently.
- Taking whiskey in a post-operative state is probably not advisable regardless of the circumstance. Hysterectomy, while relatively common, isn’t a walk in the park.
- Metronidazole can nausea and even vomiting all by itself. It doesn’t need any help from alcohol.
- See #2. 1g is a lot of metronidazole all at once, especially if you’re unused its GI effects. Would the man have vomited even if he’d not had a bottle of wine? We can’t be sure, but you can bet that it wouldn’t have been mentioned in the literature if it hadn’t. It would have been chalked up to a bad reaction to the medication.
Plosker reported a reaction following intravaginal use of metronidazole. This case involved a female pharmacist who, after two or three cocktails (each contained ~1 oz of (vodka), inserted a single vaginal suppository of metronidazole 500 mg and went to sleep. She awakened an hour later with a burning sensation in her stomach, nausea, and a severe headache accompanied by a cold sweat, which she believed was a metronidazole–ethanol reaction.
I could go for the easy ad hominem attack here, but it doesn’t serve any real purpose — and in any case, I am on my way towards showing that EtOH and metronidazole is not necessarily the End of the World. That said, the burning sensation and nausea could have been from the medication itself. Flagyl can cause this type of reaction, even when it’s not administered orally.
A potentially serious reaction involved a 16-year-old male who, nine days after resection of an hepatic echinococcal cyst, developed a staphylococcal infection. He was treated initially with intravenous vancomycin, followed by a combination of intravenous nafcillin, clindamycin, and gentamicin. This regimen was then changed to intravenous trimethoprim/sulfamethoxazole (TMP/SMX) and intravenous metronidazole, in addition to his chronic therapy with albendazole, docusate sodium, and ferrous sulfate. After 12 hours and for the following 60 hours until the TMP/SMX was switched to oral therapy, he vomited and experienced flushing, which was attributed to a metronidazole interaction with the alcohol in intravenous TMP/SMX.
Attributing these side effects to the EtOH in the TMP/SMX is easy. It’s also irresponsible, because a mechanism of action had been proposed by this point in time, but not substantiated. (Exhibit B will cover this more.) This reaction is not completely out of the question — metronidazole can indeed increase the levels of intracolonic alcohol dehydrogenase — but it’s still irresponsible to put down, for certain, that this was the cause of the boy’s distress. I wonder if the heavy antibiotics he was on could have contributed to this. It seems possible that by mowing down his normal intestinal flora, he’s in a position to experience these effects anyway.
Another potentially serious reaction reported by Harries et al. also involved intravenous metronidazole, this time combined with cefotaxime and papaveretum in a patient who had been drinking heavily and stabbed in the chest and abdomen. A chest drain was inserted and 500 mL of blood was drained; peritoneal lavage produced clear fluid only and the patient was admitted for observation. Four hours after an initial improvement, he became short of breath and nauseous; he vomited, had a headache, and was profoundly acidotic. This metabolic disturbance was attributed to a metronidazole–ethanol interaction.
Drunken guy stabbed in the chest and abdomen. Chest drain removes half a liter of fluid, and four hours later the patient complains of nausea, vomits, has a headache, and is acidotic. And then it’s attributed to a metronidazole-ethanol interaction.
I could think of a few things that’re more likely to have caused this. Can you? He’s been stabbed and he’s probably developing a hangover spring readily to mind.
This last one is a real doozy:
Toxicity due to an ethanol–metronidazole interaction appeared on the death certificate of a 31-year-old woman. Cina et al. described the case of an alcohol abuser who had been in frail health for four years following a serious car accident involving severe chest, abdominal, and closed head injuries. After being assaulted by a man, the patient had collapsed and died. Medications found at the scene included propoxyphene, acetaminophen, naproxen, metaxalone, carisoprodol, amitriptyline, hydroxyzine, vitamins, and cough syrup. No metronidazole or empty metronidazole container was found and she had not recently been prescribed metronidazole by her doctor. Because high concentrations of ethanol and acetaldehyde were found, assays were performed for disulfiram and metronidazole. There was no discussion of the methodology that reportedly found metronidazole in her serum, despite the fact that this was not one of the drugs found at the scene. In addition, there was no discussion about whether any of the other drugs in her possession, for which she was apparently not tested, may have cross-reacted in the metronidazole assay. It was concluded that she had probably ingested metronidazole without the knowledge of her physician and had discarded the bottle before she died.
I think the idiocy here speaks for itself. “It was concluded that she had probably ingested metronidazole without the knowledge of her physician and had discarded the bottle” my ass. Flagyl ain’t a drug people are likely to abuse.
Indeed the common thread throughout these cases has been the assumption that metronidazole and ethanol are the culprits without any real testing to verify whether or not this is the case. This study was published in 2000, and while there was a proposed mechanism of action for this EtOH-metronidazole reaction, there was no real evidence yet to support the proposed mechanism. There are also possible — and I would be so bold as to suggest more probable — causes for each of these adverse events, and I have done my best to explain them.
Now on to Exhibit B which talks about the science of the proposed alcohol-metronidazole interaction.
Bits and Bobs from Exhibit B (Back to top)
Disulfiram works its magic by inhibiting the hepatic low aldehyde dehydrogenase (ALDH) which increases blood acetaldehyde concentrations after alcohol is consumed. This is exactly like “Asian flush” — a common, genetic condition wherein those affected are unable to effectively metabolize alcohol completely leading to flushing, nausea, and a quickened pulse.
It was theorized that metronidazole may have a similar effect on ALDH. However, studies have shown that this is not true in rats. So, what about people?
Well, it doesn’t do it in humans, either. In fact, it had the opposite effect. Metronidazole caused a reduction in acetaldehyde production, opposite to the effect of disulfiram(!). Indeed, in Exhibit B, the graphs show (probably clinically insignificant) that the participants in the double-blind, placebo-controlled, alcohol-metronidazole study that the blood alcohol levels for the participants taking metronidazole were slightly lower than their placebo-controlled counterparts between the 40 and 80 minute marks:
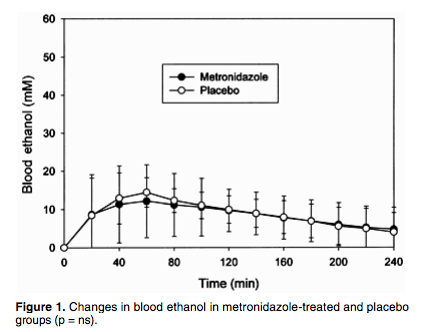
None of the participants noted any dyspnea, flushing, vertigo, or headache during the test. Interestingly, the heart rates for the metronidazole group tended to be about 10bpm lower than the control group throughout the test. I don’t know that this is clinically significant, but it is interesting:
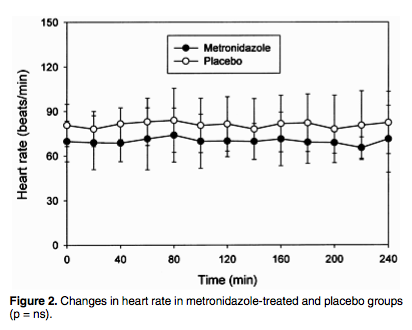
Final thoughts (Back to top)
So we’ve got some age-old advice that doesn’t stand up when tested properly, and we have a proposed mechanism of action that doesn’t hold up to closer scrutiny, either. Where does that leave us?
It leaves us with a couple things… Some people experience GI distress while on Flagyl. Sometimes they vomit. Sometimes they drink alcohol and vomit. Sometimes they drink alcohol and don’t vomit. That tells us that:
- Flagyl is hard on the stomach. It’s a difficult medication to tolerate for a good percentage of folks, regardless of its effect on blood acetaldehyde levels.
- Flagyl is not a disulfiram-like drug, and should not be referred to as such.
- Flagyl will not absolutely cause the vomiting associated with Antabuse when consumed in conjunction with alcohol. Pharmacists should stop counseling that it will.
- Adverse events are too often attributed to metronidazole because it is convenient, and “everyone knows” that alcohol and Flagyl are a recipe for disaster.
- Flagyl remains an unpleasant drug to take; its side effects are real and often severe, and should not be downplayed.
- Patients should be educated about these side effects, and how to minimize them. Avoiding alcohol is one way to do this. Taking it with food is probably more effective. Doing both is obviously better than doing just one of the two.
It is my suspicion that early researchers thought there was a link between metronidazole and alcoholism due to the medication’s side effects. Taste perversion. Smell perversion. These things will cause folks to avoid certain foods for the duration of the drug therapy. Alcohol is one of those things. It’s coincidental, and its usefulness in the real world is questionable.
When I was using Flagyl Stayed away from the drink but I did use the sanitizer (only once). I developed loads of tiny bumps on my hands where i had used the gel. After which never tried having a pint while on the anti biotics
I did not drink on the same day as flagyl, but I did drink the very next day after the last dose. I had 5 beers the next night, which is quite a bit for a woman, and I felt no ill effects whatsoever. Considering you’re supposed to take flagyl twice a day I’m guessing it has a rather short half-life. I don’t think it’s necessary to wait 3-7 days, as some suggested, after quitting flagyl before it’s safe to drink. I think it leaves your system pretty quickly.
I must say I’m amazed at how many people quit the flagyl rather than quit the alcohol to avoid the potentially hazardous mixture. So, many of you would rather endure the infection than skip a few nights of drink? What does that say about our addiction to alcohol in this world!? lol
I’m taking tinidazole, which is related to metro. Because of this they also put the fear of death in you over mixing tini with alcohol. I’m taking 500mg/day (250mg twice daily). After reading this site I decided to take a chance on the mixture. I had two glasses of wine last night. I started drinking just 1 hour after taking my evening pill. No ill effects … other than the anxiety of worrying what would happen! This morning I took my morning pill as usual, still feeling fine.
I think it’s fine that docs and pharmacists give some warning because it appears a small percentage of people do react. But I’m not sure why they like to scare the bajeebers out of us, making us fear that if we even look at a glass of wine through a restaurant window across the street that we’ll be spending the next 12 hours with our head in a toilet.
Okay…it has been a long time since I have taken Flagyl. I remember the last time drinking while on it, and only once throwing up, but honestly…it was a wild night and I really felt that it was the wild night not the Flagyl. Now many years later, I got the “not even mouthwash” speech (which I didn’t get the last time?) and kind of freaked, haven’t drank anything, but tonight is Sunday night football and who can watch their fave team without a Coor’s Light ;)? I know plenty, but I really want a few so I am going to eat, take my meds and pop open a cold one and write back later :)
I am on day 5 of a 3x 500mg Metro regiment for Clostridium Difficile or C. Diff. I seemed to have obtained it in the hospital from a stay a couple weeks earlier. (20% of cases are received that way)
I had gotten quite bored with my nearly week long sober stretch. I also had the fear of the Flying Spaghetti Monster put into me by my doctor. She said it was like “Antibuse” Assuming I would know what that was. I did. I have heard all about that before and I had absolutely zero intentions of giving that a shot. I have been feeling crappy long enough, I’ve puked plenty from drinking and I wasn’t interested in such nasty repercussions for one drunk. It looked like I had a few days left to tough it out. (One nice thing is I learned I don’t get any withdrawals or shakes as I had thought I would)
Not wanting to be sober in it’s entirety I scored 30 mg Morphine & Five 5mg Oxycodone to pass the time tonight as my Wife is out of town.
Sitting around chilling on the webs, I wanted to do some research on this whole Flagyl and Alcohol nonsense strictly out of curiosity. My initial results were fruitless. There were just a lot of the “NO NO NO DON’T DO IT!” message. It did not seem right. I finally found some stating that was a big bag of BS & then I found this site. I sat and read every single message. Mary was kinda amusing, some were just the same old shit repeating 20 others, some pointed out the obvious that we are drunks, a few had useful information.
Well, at about message 40-50 I decided to pour myself a light “Michael Phelps.” Ya know the drink, a Weed and Water. 70 Proof Sweet Tea Vodka.
My official report is that if you are me you can take 40mg Citalopram yesterday at 3PM, 2 doses Metro (last 6 hrs ago), 25mg Oxy crushed in water along with 15mg Morphine snorted roughly four hours ago, 4mg Ativan 3 hrs ago. 4 oz of total Vodka in 1.5 hours.
As of right now, I feel primo. I think I will be skipping my Trazadone here this morning.
Joe
Thank you for writing this article. I read it a few days ago and found it very informational. It calmed my fears that I probably wouldn’t die for drinking at a birthday celebration. I was a little disappointed that many commented they would follow up with their results…but did not do so. I believe the “no alcohol” rule is a BUNCH of BS and a way for the industry to CYA. I drank and was perfectly fine. Best bet is to start small, then wait and see how it goes. If anything is making you feel ill, it’s the Metronidazole! Also, I believe it’s possibly psychological. If you get paranoid and fear the side effects…then you might get sick because it’s been drilled in our heads that we would.
I commented on this post quite awhile ago and clicked the box to notify if someone else comments, so I have been keeping up with the posts and just wanted to say something else. I keep seeing people say that it is all in your head, some type of phychological response. In my case that is very much untrue. This was the first time I have ever taken the medication and I just thought that it said don’t drink because it would reduce the effects of the meds. I had no idea that it would mimic the affects of Antabuse! After spending a night throwing up like Linda Blair in the Exorcist, I crawled to my laptop and after much Googling, found this site. I can see that the majority of people haven’t had any type of reaction, so I guess I am just one of the unlucky few who cannot process both alcohol and flagyl.
Since drinking alcohol while taking Flagyl doesn’t appear to have the horrible reaction doctors and pharmacists say it does, I was wondering if this could be true of Tindamax as well. I’m on Tindamax right now and had the fear of god put into me by my doctor and pharmacist of absolutely NO ALCOHOL. Is there any information to dispute this? (Thank you so much for your information regarding this entire issue!)
It’s a bunch of bullshit. I took 4 500mg tabs today and drank 10 beers. I feel great. I’ve never paid any attention to those silly “Do Not Drink Alcohol” labels on Rx bottles. As a matter of fact, the Rx bottles with those labels are the ones you should have alcohol with. Party on.
Im on 250mg flagyl 3 times a day and last night I drank 3 wine coolers and I feel great no hangover no puking, nothing. I did get buzzed quicker but that was fine. Thanks to this website I was able to enjoy my Saturday with a couple of drinks and it felt great. This web page saved my weekend.
Well, I’ve been worrying about starting my course of Metro as it’s my birthday party om Friday and I’m at a wedding this weekend, so not drinking would’ve been horrible…so i bit the bullet and had two pints of lager this evening to see if i’m one of the unlucky ones. I’m feeling absolutely fine and dandy at the moment, so we’ll see how it goes. I’ll update tomorrow if there’s any problems.
Sorry, but your whole thesis is unprofessional and unscientific. Therefore I think I’ll continue to avoid alcohol as long as I might still have Metronidazole in my system.
If you apply Occam’s Razor it would seem that if people experience a violent reaction after drinking alcohol while taking Metronidazole, then it’s not illogical to assume that they’ve experienced a reaction to the combination of Metronidazole and alcohol.
If you want to make yourself pig sick be my guest, but please don’t encourage other people to do the same.
Chalk me up as another who has several times been prescribed flagyl but carried out drinking (moderately) with no ill-effects. I used to argue with the dentist who prescribed it because she would issue the usual dire warnings, and I would say “actually there’s no evidence” … and she would just treat me as if I was an idiot to ignore professional advice. Nowadays I just nod politely and promise not to touch a drop.
Flagyl will not absolutely cause the vomiting associated with Antabuse when consumed in conjunction with alcohol. Pharmacists should stop counseling that it will.
“Absolutely” being the key word here – meaning it’s not inevitable, but it can happen. Clearly SOME people experience adverse effects from the combination of Flagyl and alcohol. Just because it won’t “absolutely” cause adverse effects doesn’t mean it never does. Even if there’s no data, it’s still possible that some people experience it. Everybody reacts to drugs in different ways. So of course pharmacists should still warn people of a POSSIBLE adverse reaction. To not even mention it as a possibility would be totally irresponsible.
Jeez, guess I was super bored last night (have been home 3 days!) Had to test this and see for myself. I have been taking this yucky stuff for three days/500 milx2.
Built a fire, watched Elf and drank some Eggnog.
I noticed my heartbeat was a little faster, no other symptoms! I did not over do it, just a few glasses.
Merry Christmas!!!
Didn’t have time to read 266 blog entries but read enough to know it’s worth a try to “ease in” to the alcohol. Took 250 mg with breakfast, 250 mg with lunch, had about six ounces of wine with dinner, took 250 mg with a snack at 10:00 pm. ABSOLUTELY no symptoms. Today the same routine but I’m doing a vodka martini with dinner. If I’m alive in the morning, I”ll post again.
Been taking metro since 12/30 for a bout of diverticulitis. I heeded the no-alcohol warning straight through New Year’s. Yes, I spent New Year’s eve sober. But, on the bright side, I actually remember everything.
Decided to have an O’Douls (non-alcoholic) tonight with dinner. Two sips in I noticed that it actually isn’t devoid of alcohol. It has 0.5% content. Reluctantly, I stopped drinking it, opened my laptop and found this website and thread.
So, here’s my story. 1/3 of a 0.5% alcohol beer, a chicken caeser salad, and some water. 40 minutes later and my stomach is a little crampy, but it’s like that everytime I each thanks to the Cipro and Metro. No nausea, but it’s not worth it to me to risk finishing the beer. It was gawd-awful anyway. Can wait for this week to end so I can have a decent drink.
Hi there, Wow what an amazing blog.. luv it!! have to say that i have gone a week without the wine and could not leave it any longer, hence me looking up the facts on alcohol whilst on the tabs.. Am so chuffed i found this fantastic account of peoples experiances! I would like to add to it if i may..
Firstly, thank you for the person that has started this,without you we would not be able to share our thoughts etc.. well done you!!
secondly.. i have now had a bottle of wine and can normally drink at least 2 (not that i am proud about that) but tonight i am only drinking the one, i feel that its all i need.. i have the buzz feeling and feel very happy that i have so far not died..lol… i will post again to let you know if i am alive and kicking tommorrow!! i feel that on the t
abs it gives you a bit of a buzz when drinking but then i am an addictive person so please please dont take my word for it!! Do’s and Don’ts
Do’s
Think about how your affected by alcohol in general. IF you are not able to take much then don’t drink, Not because its the drink and tabs mixed but maybe you are a person that can be sick quite easily.. I am not that type of person!!! The tablets can make you feel sick on there own,, they did not with me at all, infact i felt nothing but happiness that my infection of my wisdom tooth was easing.. Thank god.. lol..
1. take tab in morn
2. make sure you eat
3. miss tab at night if you are drinking.
Dont
1. take the tablet and drink at the same time
2. drink loads and then take the tab b4 bed!! big no no!!
3. if you have reactions to tablets and can be sick quite easily then dont drink full stop!!
I can drink and can take my wine but i was sooooo worried after reading up on the facts untill i came across this blog and thought i would do a trial myself…. so far so good. infact feeling pretty good,,lol.. but in the process have realized that i must have a drink problem as i struggled to last 6 days without wine..lol.. AA here i come… and i dont mean the car brake down company..lol…
If your a hard nut then i think you will be fine but if your a sensitive person to tablets then i think you should avoid drinking..
thanks to everyone for giving me such an entertaining evening by reading your comments..
ps.. hope i dont die tonight..lol..
Love and hugs
Nicky..xx
pps. I am 33 yr old woman with 3 kids, have been on tabs for 5 days at 400mg, one, twice a day.
AA Here i come..lol.. love my wine thought… obviously!! lol
Well hello again, as you can quess i obviously did not die last night. I was’nt even sick and i didnt have a bad head. i would say that i felt a buzz and a bit drunk quicker than normall but thats it!
Least i know now..
thanks again and will go get a large glass of wine as its saturday night… yeay!!!
xx
Reading this was hysterical….I feel just like most of you..Last Flagyl an hour ago. Refrained from drinking the last 7 days and SHIT,,,,what a complete nightmare…I feel as if I may need AA now..Can’t WAIT to drink tomorrow and I can’t believe I made it 7 whole days freaking out..Cranky 33 yr old sober bitch I was for sure..Hoping not to get any bad reaction tomorrow..doubtful..Good luck to you all !!!!
I took my first dose today around 6pm with dinner. I felt a bit nauseous about 30 minutes later, but my stomach soon calmed down. I’ve had a bad cold for the past few days as well, and have been so exhausted, so I wanted something to knock me out tonight. Without even thinking, I took some NyQuil. As soon as I did it, I paused, and nearly smacked myself in the forehead, since it has alcohol with it. However, I feel fine (apart from the NyQuil making me sleepy!) and reading this article soothed my nerves. I plan to avoid alcohol while on this medication, but I can’t imagine taking such a small amount is that bad for you.
Ok ok. You’ve convinced me. I’m going to enjoy my dinner with some wine, see how I feel from there. And then go out and party all night. Thank you for clarifying, I cannot wait any longer to go out and drink (I am a college student who’s missed out on a lot of parties during my dosage). If however I do get sick..there will be a mch meaner blog tomorrow morning..just kidding. Thanks again for your informative post.
Ok, I originally had read this entire thread because I was worried about whether or not I would be deathly ill from consuming a few drinks while taking Metronidazole. Here’s some info first: I am taking 500mg every 12 hrs for a week. I am female and weigh about 155 lbs. Because I had no idea how the alcohol would affect me, I decided to take it reallllly slow. So i started by having just one drink (one shot of vodka mixed with diet coke) an hour. I did this for two hours, then took my pill (with a small granola bar) and then had a drink right after taking the pill. I felt no ill effects and certainly was not drunk at all. So you can definitely drink when taking this antibiotic, just don’t drink as much as you usually do thinking you will get hammered as usual–I’m sure if I were to have drank more in a shorter amount of time I just would have gotten drunker faster.
A common theme running through many of the posts is the huge over-consumption of alcohol, whether or not on Flagyl.
It’s good to know that one can enjoy a drink or possibly two while taking Flagyl, however many of these posts indicate alcoholic drinking patterns i.e. throwing away a beneficial antibiotic so they can drink large amounts of alcohol.
I do appreciate the thoughtful and analytical article. Too many times, medical professionals, as well as the general public will pass on anecdotal information for so long that it turns into “we all know”. Yes? Based upon?
good summary of the evidence out there..
I am female, 21 years old, 165cm (approx 5’6”), 54kgs (approx 123 lbs) have possible pseudomembranous collitis and have been prescribed 400mg metronidazole x3 a day.
I am an antibiotic warrior. I have been on a few rounds of Keflex the last few months for reoccuring folliculitis. Apart from that, I’m quite healthy.
I wasn’t warned emphatically about taking alcohol at all with this antibiotic. But I noticed the pharmicist had gone to the extra trouble of adding her own warning label on the side of my bottle so of course…straight to google.
It’s my 21st party this weekend. I’m not going to drink heavily at all..but I intend to have a few glasses of bubbly with my friends considering ive been organising it for so long..hopefully my results concur with the majority of the other posters in regards to tolerance. Will post up Sunday morning!
With not feeling well for a couple of weeks, eventually causing enough of an issue to require a doc visit; I was diagnosed with BV. The PA prescribed metro gel, one dose inserted nightly for 5 days. One health concern slightly improved, but I continued to fall more and more into ill health (fever, aches, chills, fatigue, and overwhelming awful feelings like a severe flu). In calling the PA for follow-up, they then prescribed the metro pills (generic), 500mg twice a day for 7 days.
I was heavily warned not to drink any kind of liquor from the nurse and the pharmacist, but, nothing so far as not swishing mouth wash or using hand sanitizers. lol And strongly told to eat with each dose! I have made sure to eat yogurt and fill my tummy to protect it from GI repercussions. I am flowing right along while taking these, with no major side issues to report. :) <>
In my daily routine, I drink a couple/few cans of beer – continued through-out the gel treatment with no ill effects. And with the pills, I continued to have a few beers; but, changed to a couple of stiff vodka drinks last night. I am feeling a bit woozy/drowsy this morning, but, I know it will fade away sooner or later.
I don’t know if it was because of the vodka drinks and getting too much of a buzz combined with the pills or not. More than likely, it is the infection leaving my body; and having been so ill for far too long, that my body has much further to come back to being healthy.
Also that I am now more dehydrated than “normal” with the vodka and taking these strong pills — that alone can cause the woozy feelings.
So, be sure to drink water, lots of water, and keep it going long after you end the medications. Help keep your system fresh flowing, detoxify, and aid in healing.
I ended up in the hospital last week after throwing up for a few days. It started out every few hours, but by day three I was throwing up constantly and when I began puking blood I went to the ER. I ended up being admitted for three days. Turns out I have many stomach ulcers and a bad UTI. I was given Metro by IV for three days and when I was discharged was given a scrip for Metro 500mg three times a day. I was given a packet of info about mixing alcohol and Metro the first day I was in the hospital. I just stuck it in my bag and forgot about it. Well, yesterday was Valentine’s Day. I live in Phoenix and it is in the upper 70’s. So, I told my boyfriend I wanted to lay by the pool and drink pina coladas. Plus, my “snowbird” neighbors from Canada, who drink everyday, were having a little party on their patio. Why not?, They are retired, they deserve it. Anyway, I remembered getting that paper about one of my meds, so I pulled it out and read it.
Well, you all know, they put the fear of death in you, no mouthwash, cough syrup etc… Plus the pharmacist warned me to absolutely NOT drink alcohol with it. I was really worried! I did take Antabuse when I was a teenager to make my parents chill out. So, I did know what could happen. Anyway… I pulled out the laptop and came across your informative and amusing site. My boyfriend and I said this is cool, just start slow and see what happens. Well, I hung out by the pool, drank my frozen drinks, then partied with the Canadians. Not a thing happened to me except I had a great time. My boyfriend on the other hand, who is not on meds, got completely wasted and hit about every wall in the house and landed on the kitchen floor! I could only laugh. One thing I did do was stay away from the strong vodka soda’s which I normally drink.
So, thank you for your great information. Because of you I had a great V-day, just not a happy ending, thanks to the boyfriend (;.
Take care
i took metro 2 hrs ago, and now finishing second bottle of beer. nothing happened so far
Was on 200mg t.d.s Sat-Wed for gum infection. Like many others avoided mouthwash (JUST when I needed it, argh) and had the last pill at 9pm last night. No stomach upset whilst on them, as warned by dentist, and things orally have cleared up a treat.
Have something to celebrate with the BF so got some Chardonnay (yes, another Bridget Jones *sigh*) and it took about 20 mins of staring balefully at a glass of it before I came across this site, prostrated myself before the genius of the OP and took the plunge.
Halfway through glass one, flushed cheeks (hardly surprising after a week off the sauce) fear of vom receding. Will post again tomorrow.
Alrighty….after being on two antibiotics for about a month now, flagyl and augmentin for a non ending dental nightmare, I had a few friends flying in for a reunion. Although a little hesitant at first, I decided to throw caution to the wind and celebrate my friends being in town. I figured I’d start out with one drink and see how I felt. NY Presbyterian was close enough in case of emergency. One goose and soda…fine. Two, three, four…I was FINE!!! It’s the next dayI think it either just effects a very small percentage or it’s the placebo effect that causes the reaction. Who knows…no effect on me. I will DEF be enjoying a cocktail with brunch this weekend :-)
Flagyl 500 mg 2X day. Didn’t take evening dose for Easter party last night. 1/2 bottle of champagne, 1 bloody mary and 5 or six beers. All over a 6 hour period. I felt fine the whole time and it’s the morning after now; feeling great! Thanks everyone.
I am taking the Metro 400mg x 3 a day as well as Amoxicillan. Got the heavy alcohol warning from the Doc and the Chemist. 2nd day on tablets, went out last night for dinner last night and shared a bottle of wine with my bf followed by a shot of sambuca with a short black coffee – no ill effects whatsoever. I got a bit gutsy after reading all the posts on this site, thanks by the way bacuase I like my wine with my meals. I just made sure I took all the doses of Metro by 4pm as my dinner was at 8pm. Just to be cautious I didn’t have my wine until food was served, whether this helped or not is unknown. Will be having drinks tonight aswell!!
I´ve been in metro for the last 5 days, 3x400mg. Friday morning, 7am i had my last pill. I didnt have any side effects at all to be honest, just pain in my gum which was the reason i was taking it for in the first place. I was pretty scared about the alcohol mixing thing, but after reading all these comments im gonna give it a go, considering i have a house party tonight at home. I´ve been drinking water all day long to get it out of my system as soon as, gonna have a heavy dinner and then pace myself with the beer, i will let u know tomorrow guys, cheers everyone for sharing the experiences!
Juan again. Well its the next morning, and i had beers all night without a problem. Maybe a weird feeling at first in my hands, and a slight headache, but i think it was my imagination more than anything else. Lucky me then!
Ok I’m on 400mg 3x a day for 7 days. I’m currently finished my 5th day. My last tablet will be Wednesday morning. A friend of mine is heading off to Australia for a year or and she is having a going away party and I’ll be damned if I’m the only one in a crowd of maybe 50 people not drinking. Working it out it will be able 62 hours before I drink so I should hopefully be fine.
I was told not to EVER mix with alcohol, so I’m glad I found this. I was prescribed Metronidazole 500 mg twice a day for 7 days. After reading this, I went out this weekend and had 2 drinks and I felt fine the next day, no throwing up. I took the evening tablet 3-4 hours before my first drink. I have 3 more days to go, can’t wait to be done. Hope this helps, good luck!
I work in the Pharma industry. Pharma will NEVER take off an old warning, regardless of the facts. Given the state of the law, there is no reason for them to. If they remove the warning re alcohol and Metronidazole and some bizarre set of fact occurs as outlined in the article above, the company can be found liable by a jury and have to cough up a good chunk of change. Thus, to a pharma company there is no harm leaving the warning and possible harm from removing it. What would you do?
Unfortunately, this leaves a good deal of misinformation. As for the 3 day rule, I can now personally attest that it is complete crap!
I drank all night on flagyl… just felt normal abx stomachache is all… actually a little worse than normal stomachache but i expected that drinkin or not
Just took 500mg pill today and drunk 1 whole 5th and a half of vodka…I have been vomiting for the past hour do not drink with alcohol is righttt!I followed these jerks advice on this website and look at me now!Im literally typing in my own puke.F these lying bastards.
Umm, Bill, could you be throwing up due to the fact that you drank a whole fifth and a 1/2 of vodka in one sitting? That just might have something to do with it. I’m just sayin’…..
Work in the med field and was put off by the non-option of alcohol with flagyl. Went 2 days without anything and found this site. Had a 2 beers with an hour, no ill effects. Went out for dinner with girlfriend and shared a bottle of wine. So far so good. Took another 5oo mg before bed as prescribed. Don’t skip your dose!
Will follow-up tomorrow.
Woke up with non for wear. Pretty typical morning after night of drinking 2 beers and a shared bottle of wine.
This is a great and very enlightening website!
Thank you so much.
Enjoyed going through this site.
I too have been prescribed Flagyl and have been reluctant about starting it because of the alcohol issues.
I’m an RN so I am aware that we tell patients things sometimes that are in their best interest but probably are not backed up by fact.
I had been feeling this way about Flagyl and alcohol.
Any research I did resulted in many warnings but no obvious science behind them.
Based on this,my need to take a 10 day course of Flagyl, my desire to continue to drink while doing that and what I’ve read on this web site my experiment has begun.
I have already had a couple of glasses of wine, I just washed a 500mg Flagyl down with a third, I plan to have at least a few more tonight.
Update in the am.
Wish me luck.
Alan,
I haven’t posted for awhile because I’ve been off Flagyl since I started Opium (thank you group for the suggestion). The key to alcohol and Flagyl is MODERATION. Alan, taking your Flagyl dose with a third glass of wine just makes no sense. I enjoyed the occassional Martini while on Flagyl with no symptoms but I timed my drink away from my dose and I didn’t have multiple drinks. C’mon, use your head.
barry
Thanks Barry.
Much Opium tonight yet?
Seems like a good replacement for alcohol and Flagyl.
That’s not illegal in your state?
Still good here,no vomiting etc and with it enough to be annoyed by an idiot like Barry.
Case closed.
Your still talking Barry….have a litle more Opium and STFU.
Regards
Bedtime Flagyl coming up.
More to follow.
Alan,
Tincture of Opium is an old fashioned medication that is coming back into favor. It’s a class 3 narcotic that can be difficult for pharmacies to get. I’m surprised with a nursing background you were not aware of this. It does not give you a high but reduces the pain and spasm in the gut and people never get nasty while they take it. It’s obvious you are new to the site and you will find no one gets insulting unless they’ve had too much alcohol with their Flagyl.
barry
LOL Barry
As new as I may be to the site it does not appear to be a forum for unsolicited commentary on the drinking habits of others in yet you choose to use it this way so I’ll stick with my STFU thanks.
That said, I experienced none of the promised perils of mixing alcohol and Flagyl.
I plan to continue to drink during the course of Flagyl.
Update to follow.
I’ve been drinking in moderation for several days now with little ill effects. I’m feeling the same hangover whether I was taking flagyl or not.
Didn’t want to give the impression I couldn’t go without alcohol for a couple days! That is definitely not the case at all. In fact I go months without it, I am however on vacation which is ending for soon!
Thanks again for this very informative and enlightening site!
Closing the loop.
Drank my way through 10 days of Flagyl 500mg TID without any obvious side effects or discomfort.
Based on my very limited study, my opinion would be that the Flagyl/alcohol warnings are grossly over-stated.
That said, always follow doctors orders.:-)